Demystifying IRMAA Appeal: Just How It Functions and What You Required to Know
The IRMAA appeal procedure can commonly appear discouraging for Medicare recipients facing unexpected premium increases. Understanding the intricacies of IRMAA and its influence on expenses is important. Lots of people may not recognize they have the choice to appeal these modifications. By discovering the factors behind these charms and the required steps, beneficiaries can possibly relieve their economic worry. What specific approaches can one use to browse this complicated system efficiently?
Understanding IRMAA: What It Is and That It Affects
IRMAA, or Income-Related Monthly Adjustment Amount, is a critical part of Medicare's prices structure that influences recipients based on their income degrees. Presented to make sure that higher-income individuals add more to their healthcare expenses, IRMAA modifies the typical premiums for Medicare Component B and Component D. Beneficiaries with incomes above certain limits may face increased costs, which can substantially impact their total health care costs.
The change puts on people and pairs, considering their changed adjusted gross earnings from two years prior. This suggests that those who may have experienced a decline in earnings might still deal with higher premiums based upon past incomes. Understanding IRMAA is necessary for recipients as it can affect their monetary planning and medical care decisions. Understanding of this change helps individuals navigate their Medicare choices more successfully, guaranteeing they are prepared for the prospective expenses linked with their coverage.
How IRMAA Is Determined: Earnings Limits and Changes
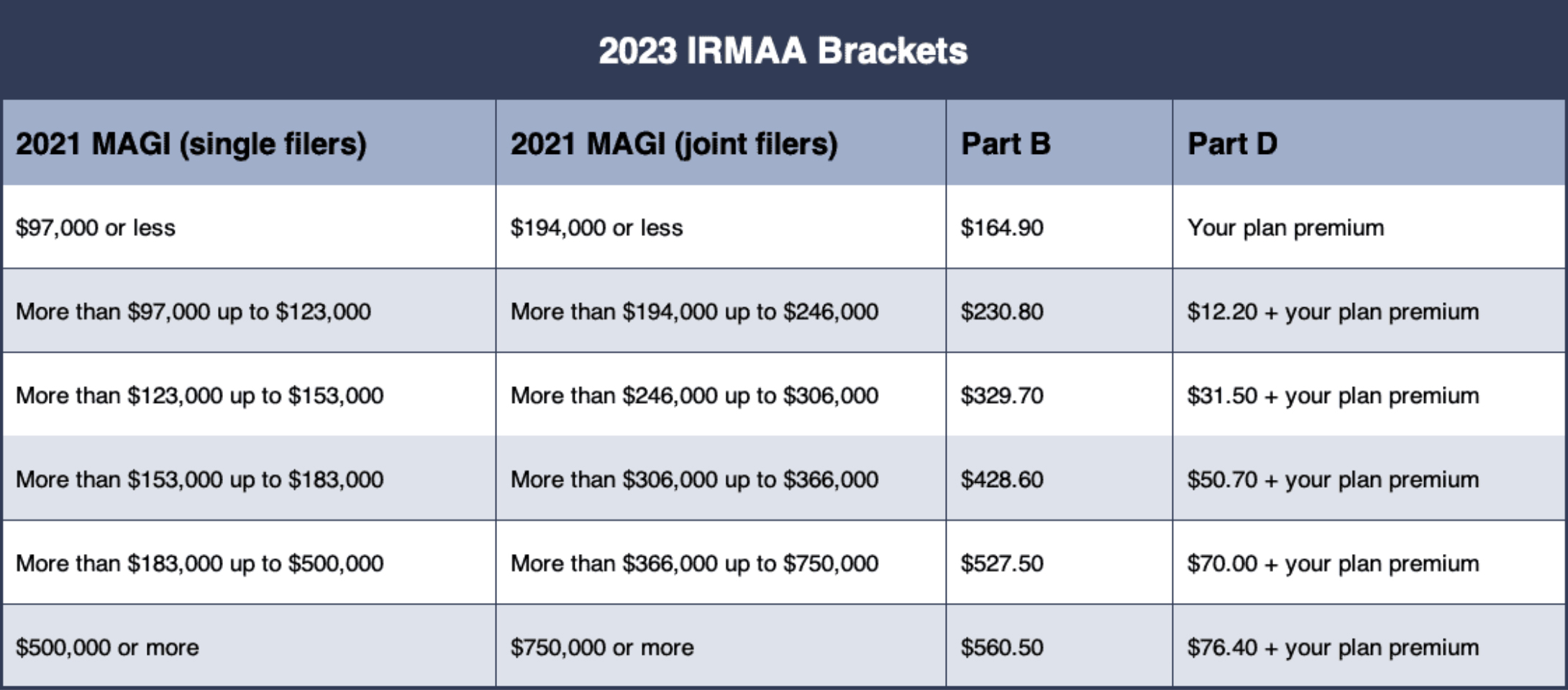
Calculating the Income-Related Regular monthly Modification Quantity entails specific income thresholds that determine the extra costs for Medicare recipients. The limits are readjusted each year and are based upon the recipient's modified changed gross earnings (MAGI) from two years prior. For instance, in 2023, individuals with a MAGI surpassing $97,000 and pairs going beyond $194,000 might sustain higher premiums.
The Income-Related Monthly Adjustment Amount is tiered, meaning the costs raises as revenue increases. As an example, those with a MAGI in between $97,001 and $123,000 will pay a certain additional amount, while those exceeding $500,000 encounter the greatest surcharges.
These adjustments guarantee that higher-income beneficiaries add more toward their Medicare expenses. Understanding these thresholds and changes can assist recipients anticipate their costs and intend their finances appropriately, guaranteeing they are not caught off guard by prospective increases in their month-to-month Medicare costs.
Usual Factors for IRMAA Appeals
Many recipients may find themselves dealing with an unforeseen IRMAA analysis, leading them to take into consideration an appeal. One typical reason for such appeals is a considerable life adjustment that affects income, such as retirement or work loss. Recipients might argue that their present income is reduced than what was reported to the IRS, thereby validating a decrease in their IRMAA.
Another regular factor involves inconsistencies in noted income, where individuals think that their revenue was incorrectly analyzed due to mistakes in tax obligation returns or financial files. Furthermore, some recipients might appeal based upon unique situations, such as the death of a spouse or find out this here major medical expenditures that have affected their monetary situation. Comprehending these usual factors can empower beneficiaries to present a solid situation when browsing the IRMAA appeal procedure effectively.
Step-by-Step Guide to the IRMAA Appeal Process
Navigating the IRMAA appeal process look at here now can be complicated, yet recognizing the actions entailed can simplify the journey. The very first step is to gather relevant documentation, including tax returns and proof of income modifications. Next off, individuals should complete the appeal form, which can normally be found on the Social Safety Management (SSA) website. This kind should be submitted within 60 days of obtaining the IRMAA resolution notice.
Once the appeal is filed, the SSA will certainly examine the info offered and may ask for added documentation. It is important to keep duplicates of all sent materials for individual documents. After the testimonial procedure, the SSA will certainly provide a decision, which will be communicated in composing. People have the choice to request a hearing prior to a management law judge if the appeal is rejected. Throughout the process, maintaining arranged documents and adhering to timelines can significantly boost the chances of an effective appeal.

Tips for an Effective Appeal: What You Required to Know
An extensive understanding of key methods can substantially boost the probability of a successful IRMAA appeal. Initially, it is vital to gather extensive paperwork, consisting of tax obligation returns and any type of appropriate monetary statements. This evidence sustains the case for a decrease in income-related month-to-month modification amounts. Second, individuals should understand the specific scenarios that certify for a charm, such as considerable life changes-- retired life, special needs, or loss of earnings.
Third, sending the appeal within the stated timeframe is vital; missing out on due dates can result in automated rejections. Additionally, crafting a clear, concise letter that lays out the reasons for the appeal can enhance its performance. Persistence is crucial, as the testimonial process might take time. By adhering to these standards, people can considerably strengthen their possibilities of accomplishing a beneficial end result Extra resources in their IRMAA appeal.
Often Asked Questions

Can I Appeal IRMAA Decisions Several Times?
If they supply brand-new proof or an adjustment in conditions, people can appeal IRMAA choices several times. Each appeal should be corroborated with appropriate documentation to support the request for reconsideration of the decision.
How much time Does the IRMAA Appeal Process Take?
Will My IRMAA Appeal Influence My Medicare Coverage?
The IRMAA appeal does not influence Medicare insurance coverage. It exclusively addresses income-related adjustments to premiums. Beneficiaries preserve their insurance coverage throughout the appeal procedure, guaranteeing continuity of medical services while awaiting the result of the appeal.
Exist Any Type Of Costs Linked With Filing a Charm?
Submitting a charm commonly does not incur direct fees; nevertheless, connected expenses may occur from required documentation or lawful assistance - irmaa brackets. It is suggested to validate certain demands and prospective costs with the pertinent Medicare workplace

Just how Will I Be Notified About the Appeal Decision?
Individuals will obtain notification regarding the appeal decision using mail. The choice letter will lay out the outcome and give more guidelines if required, making certain that the individual is educated regarding the next actions to take.
The IRMAA appeal procedure can usually seem daunting for Medicare beneficiaries dealing with unanticipated costs increases. Numerous recipients may find themselves encountering an unforeseen IRMAA evaluation, leading them to think about a charm. Navigating the IRMAA appeal process can be daunting, however recognizing the actions included can simplify the trip. Individuals can appeal IRMAA choices multiple times if they give brand-new evidence or a change in circumstances. The IRMAA appeal process usually takes about 60 days from the date of entry.